Kathy Myburgh, Ph.D., FACSM, is a distinguished professor and the South African Research Chair in Skeletal Muscle Physiology, Biology and Biotechnology at Stellenbosch University and leader of the Muscle Research Group, which specializes in muscle damage and repair. The 2023 recipient of a Citation Award from the American College of Sports Medicine was nominated for the award by Bruce Gladden, Ph.D., FACSM.
Early life
Gymnastics was Myburgh’s entrée into the world of exercise science. Though she began her career relatively late for a competitive gymnast — she started training at the age of 11 — she was both talented and persistent. Which has its rewards. The South African-born Myburgh would go on to join the national gymnastics team, competing as a high-level athlete from the late 1970s though early ’80s, including against eventual U.S. Olympic Gold Medalist Mary Lou Retton when Retton was the USA Junior Champion and sent to South Africa to gain travel experience under rather different conditions.
The natural tenacity of a competitive gymnast acquits itself well in the world of research. Myburgh notes that the mindset required of both the elite athlete and the serious researcher is the fundamental acceptance of slow, meticulous progress combined with a tolerance for questioning lack of progress. I ask her to explain the driving force behind this acceptance.
“That’s easy,” she says. “It’s worth it.”
Undergraduate work
Myburgh would first enroll, on a gymnastics scholarship, in a bachelor’s program at the University of Pretoria focusing on both physical education and English literature. South African baccalaureate programs consist of three years of study capped with a research-intensive honors year similar to the coursework of an American master’s program. During this latter portion of her undergraduate studies, she transferred to the University of Cape Town to study under Professor Tim Noakes (essentially the progenitor of sports medicine in South Africa) and his team, where she specialized in exercise physiology and related subjects like exercise biochemistry and biomechanics. She produced her debut paper, which assessed the effectiveness of athletic taping (a then relatively novel approach to the maintenance of joint stability) versus that of ankle guards in racquetball players.
For this, she used a recently developed electronic goniometer — a device that measures ankle flexion, and was the first person to employ this electronic version instead of a traditional model, which looks something like the chimeric offspring of a carpenter’s square, draftsman’s compass and primary school protractor.
The paper has been cited 88 times, the last two citations having been for book chapters in 2021 and 2022, respectively.
Master’s and Ph.D. studies
After earning her bachelor’s degree, Myburgh spent a year as a high school teacher before deciding return to the University of Cape Town to pursue master’s studies, later transitioning into a Ph.D. track. It was here she began her formal study of the musculoskeletal system, which would be the focus of her career.
While still in the master’s portion of her studies, Myburgh was working in a calcium lab that studied osteoporosis. It was the early 1980s. At the time, she says, exercise wasn’t considered an appropriate intervention for skeletal issues; prescribed physical activity was really something that cardiovascular researchers had an interest in. However, studies from Scandinavia soon showed a difference in bone density in the forearms of professional tennis players; the bone was, of course, denser in the dominant forearm. This gave Myburgh and others the confirmation they needed to pursue the effects of exercise on the skeleton.
“I did a study on rodents and induced osteoporosis as a model and had them run as a prevention,” she says. “That was twelve months — my little rats had to run five times a week on the treadmill. And it prevented the bone loss.”
The paper was published in the Journal of Applied Physiology.
“This is work I’m really proud of,” Myburgh says, though she cautions that the research has moved on since her study. “That is the work that got me noticed at the American College of Sports Medicine — the first project on the rodents and osteoporosis I presented at my first ACSM meeting.”
When she transitioned into a Ph.D. track, Noakes became her mentor. As part of their studies, Myburgh and her fellow students attended a running injury clinic held each Monday, and one of the topics covered happened to be stress fractures. This raised some questions in Myburgh’s mind.
At the time, the prevailing view was that stress fractures were primarily caused by imperfect biomechanics and improper training modalities, particularly overtraining. However, as an athlete, Myburgh had experienced shin splints and seen fellow competitors suffer from stress fractures. And her experience studying osteoporosis in mice suggested to her that exercise, at least in appropriate amounts, should be protective rather than the cause of bone injury. This opened up a line of inquiry for her doctoral studies:
“Linking these things, I could do some research for my Ph.D., which then showed that amenorrhea is a risk factor for shin splints — that was the first study. But the main study, the seminal final chapter of my Ph.D. — South Africa had two bone mineral density machines and one of them was at Grootte Schuur hospital (the Cape Town hospital where the first heart transplant was done), and I was at the University of Cape Town, so we could actually measure the bone mineral density (BMD) of these relatively young people getting stress fractures. This had never been done before. … I found that if you took athletes of the same sport, and if they were runners, the same racing distance, and matched for training distance, those with a history of menstrual dysfunction and low calcium intake were more likely to have stress fractures, even when their biomechanics was normal. Important was that their BMD was lower than the athletic controls without stress fractures.”
The study was published in the Annals of Internal Medicine and has been cited 340 times since 1990. This work, among other of her efforts, which focused on middle-aged athletes who had experienced amenorrhea earlier in life — prefigured the female athlete triad.
Postdoctoral studies; Stanford and UCSF
 After completing her Ph.D., Myburgh became a postdoctoral researcher at Stanford, joining the Division for Geriatric Endocrinology because of her bone expertise. It was while at Stanford she became an ACSM fellow (1991). It was also there that she met a Ph.D. student who was looking into low muscle mass in older people, thus reinvigorating her interest in the muscular side of the musculoskeletal equation.
After completing her Ph.D., Myburgh became a postdoctoral researcher at Stanford, joining the Division for Geriatric Endocrinology because of her bone expertise. It was while at Stanford she became an ACSM fellow (1991). It was also there that she met a Ph.D. student who was looking into low muscle mass in older people, thus reinvigorating her interest in the muscular side of the musculoskeletal equation.
Though she had always been interested in both bone and muscle, Myburgh hadn’t had the opportunity to specialize in the latter during her Ph.D. After Stanford, she would complete a second postdoc, this time at the University of California San Francisco medical center. It was there she had an opportunity to make the transition into muscle research. Beyond her direct interest in the subject, there were also practical incentives:
“Muscle is more responsive (than bone) in a shorter period of time,” she says. “With studies on muscles, the study duration itself can be quite a bit shorter. You can get more done.”
Thus began her work studying single muscle fibers — including measurements of contractile force and velocity — sourced from the (conveniently long) psoas muscle of rabbits. The chief purpose was to understand which of the molecular changes one observes in fatigued muscle tissue would prove to be influential when tested individually in a single muscle fiber.
South Africa and Stellenbosch
But having spent four years in the U.S., Myburgh returned to South Africa, again working with Noakes at the University of Cape Town, this time studying muscle adaptation, via biopsy, particularly during high intensity training, which was gaining popularity at the time.
By 1997, she had accepted a tenure-track senior lecturer position, the South African equivalent of an assistant professorship, at the University of Stellenbosch. She has remained there to this day, eventually rising to her current position as distinguished professor, the highest achievable title at said institution.
Over the course of her career, Myburgh has authored over 180 publications, receiving nearly 15,000 citations, and has an h-index of 38. Beyond her work with bone, amenorrhea, and muscle fatigue, she has also studied the differentiation of muscle fibers and how differential training produces differing competitive results, particularly when it comes to, colloquially, fast-twitch and slow-twitch fibers.
During that time, she has also been extensively active with ACSM.
Says Myburgh, “The ACSM has always been what I call my Academic Home Society. I have attended around 20 ACSM conferences over the years. I met wonderful people in my field of interest whose respect for my work encouraged me. I was happy to contribute to the ACSM Annual Meeting Program on occasion when I thought I had something interesting to share.”
Contemporary efforts
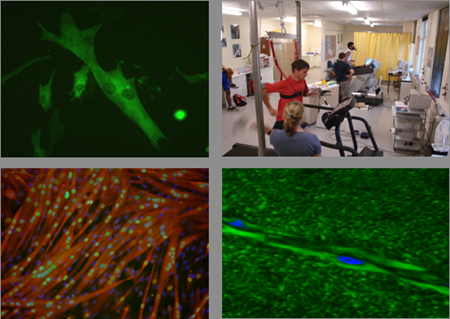 Myburgh’s current research is stepping into what may very well be a wide-open field of discovery. As leader of Stellenbosch’s Muscle Research Group, she heads up teams studying, broadly, two related realms: satellite (stem) cells called myoblasts, and small extracellular vesicles — particularly exosomes. The work takes place both at the bench and with human volunteers.
Myburgh’s current research is stepping into what may very well be a wide-open field of discovery. As leader of Stellenbosch’s Muscle Research Group, she heads up teams studying, broadly, two related realms: satellite (stem) cells called myoblasts, and small extracellular vesicles — particularly exosomes. The work takes place both at the bench and with human volunteers.
Myoblasts. Myoblasts are stem cells located around muscle tissue that are able to step in, so to speak, when the muscle is damaged. They do so via a number of methods: by (a) secreting helpful molecules or, as recently discovered, exosomes; (b) migrating to the injured fiber and incorporating themselves into it — by fusing cell membranes and then introducing their nucleus into the damaged fiber, itself essentially a very long single cell with multiple nuclei; and (c) multiplying and fusing themselves together to form an entirely new muscle fiber if the damage is extensive enough to require such action.
One of the study modalities involves placing muscle cells in a multi-well culture dish, then creating an artificial injury by creating a division between cells in two halves of the well and observing the myoblasts as they inchworm their way across the well using structures called lamellipodia in order to fill the severed section.
(An aside: Lamellipodia don’t adhere well to plastic, so the researchers must first coat the wells with a substrate in order to give the cells “grip,” so to speak.)
“We can do this with time-lapse microscopy,” Myburgh says. “So you take images at time intervals to watch the myoblasts migrate into the gap and close the gap.”
Exosomes. Exosomes, on the other hand, are nanovesicles produced within cells, in this case muscle fibers and myoblasts, that are released into the blood stream and may communicate information about an injury, about necessary whole-organism responses to exercise — frankly, we don’t yet know all they do. Which is particularly interesting because the process of vesicle production is quite old, evolutionarily speaking, and therefore common to many seemingly disparate organisms:
“Even plants, also yeasts, they all make vesicles,” Myburgh says.
At the moment, one of Myburgh’s graduate students is trying to determine whether myoblasts accept into themselves exosomes that the researchers source from volunteers’ blood plasma.
As to the exosomes’ formation:
“These vesicles are actually purposefully synthesized, first into a bundle of vesicles intracellularly which is called a multivesicular body and that goes to the (cell) membrane and releases a whole lot of vesicles together … and this purposefulness is why the cargo is so important,” Myburgh says. “Because whist the muscle is purposefully creating these vesicles and gathering them in a multivesicular body, they can put in, the cell can theoretically put in what it would like to put in — or what is prominent in the cell environment at the time, is a better way to say it.”
The opportunities in this area seem boundless. For instance, do the signatures within exosomes differ depending on whether said exosomes were produced by newer or older muscle cells?
“They could potentially become biomarkers, and biomarkers for the state of the muscle,” Myburgh says.
Primarily, though, she and her team are focusing on identifying exosomes produced by muscle cells that are damaged.
The future
Thus, when I ask what’s the most exciting question for her, she offers:
“The question that we have is related quite a lot at the moment to the (exosomes’) cargo. So if you induce damage in a human volunteer, for example you make them do a lot of plyometric jumping or downhill running on the treadmill and they end up with muscle soreness the next day from unaccustomed exercise, and we’ve drawn out blood samples at various time points, can we determine if the cargo has in fact changed? Can we separate out the vesicles that originated from muscle and those that originated from other cells? Because in circulation, (extracellular vesicles) are common …
“This is something that is also a burning question in the field — how to identify very clearly which of the vesicles of the billions you get out of 20 mL of blood, for example, or 1 mL of plasma, which of them actually came from muscle. This a burning question which will then help us answer the physiology questions.”
In closing
Fascinating things are afoot, and there is much progress to make.
Myburgh’s students have a wide open field before them. And she is incredibly grateful to them:
“I couldn’t have done any of this without all the students who have been part of my Muscle Research Group … I’ve had postdoctoral fellows local and from the USA, Canada, United Kingdom and Europe; Ph.D. students; master’s students, all of them working very hard, and they achieved this with me,” she says.
Several have gone on to become full professors in their own right.
As Myburgh puts it: “It’s very exciting to be in this timeframe.”