Kenneth Powell, M.D., MPH. FACSM |
Aug.
16, 2019

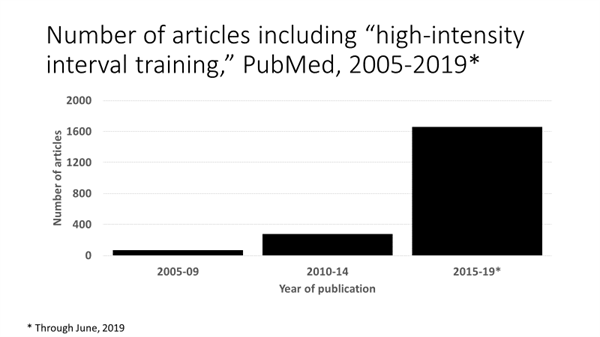
That which was old is new again. High-intensity interval training (HIIT) has been a common component of exercise regimens designed to improve fitness and performance for many generations. In recent years, research interest has surged. A simple search of PubMed for the term “high-intensity interval training” reveals a more than 20-fold increase in the number of hits between 2005-09 and 2015-2019. The increase is due to the possibility, rather likelihood, that HIIT provides health benefits in addition to fitness benefits. The
July 2019 issue of
Medicine & Science in Sports & Exercise (MSSE) alone included four articles reporting investigations of the relationship between HIIT and health indicators.
The 2018 Physical Activity Guidelines Advisory Committee (PAGAC) recognized the importance of the relationship between HIIT and health and included an umbrella review in its final Report. The search was updated, and the write up was revised and included in a Special Communications section of the June 2019 issue of MSSE as High-Intensity Interval Training for Cardiometabolic Disease Prevention. The PAGAC Report and the article conclude that HIIT improves insulin sensitivity, blood pressure, and body composition equivalent to the improvements provided by moderate-intensity continuous training.
The basic structure of HIIT is generally understood – short periods of high intensity exercise alternating with usually longer but still brief periods of lower intensity exercise. In practice, however, the format varies considerably. The duration of bouts of high intensity, the duration of periods of recovery, the specific intensity of high intensity, the specific intensity of the recovery periods and the number of cycles vary.
HIIT deserves the resurgence of interest because HIIT-related research, using device-measured physical activity, can refine our understanding of the relative importance of frequency, duration and intensity of physical activity. The prevailing conclusion, based largely upon self-reported physical activity, is that total volume of moderate-to-vigorous physical activity (MVPA) – the product of frequency, duration, and intensity – is more closely related to health benefits than any of the three components. The prevailing conclusion may, indeed, prevail. But HIIT research in which frequency, duration, and intensity are varied may provide new insights. HIIT research may even be able to contribute to our understanding of the health benefits of light intensity physical activity as well as very short episodes of MVPA.
The acceptability of HIIT regimes also deserves more study. The best physical activity regimens are the ones that people can and will continue to do over the years. Adherence to HIIT over time, as well as when and for whom HIIT is appropriate remains to be determined. In addition, the rates of musculoskeletal injuries and other activity-related adverse events are likely to be higher than for activity at lower intensities. Risk of injury is directly related to size of the physiologic overload, that is, the size of the increase in volume or intensity. Although the reputed injury and drop-out rates from HIIT have been small, the populations have been small and selective, and follow-up periods have been short.
The currently high level of interest in HIIT provides us with opportunities to explore many important and interesting physical-activity related questions. I’m glad it’s back!
Learn more about the Physical Activity Guidelines for Americans, 2nd Edition
 Kenneth Powell, M.D., MPH. FACSM, was an epidemiologist with the CDC for 25 years and with the Georgia Department of Human Resources for 8 years. He is now retired and lives in Atlanta. The relationship between physical activity and health has been an important theme during his career. He planned, chaired, and edited the papers from the first national workshop on the epidemiologic and public health aspects of physical activity and exercise in 1985. Dr. Powell served on the Institute of Medicine Committee on Physical Activity, Health, Transportation, and Land Use (2005); Committee on Progress in Preventing Childhood Obesity (2008); and Committee on Physical Activity and Physical Education in the School Setting (2013). He was a member of the 2008 Physical Activity Guidelines Advisory Committee and a co-chair of the 2018 Physical Activity Guidelines Advisory Committee. He is a graduate of Harvard College, Northwestern University School of Medicine, and the Harvard School of Public Health.
Kenneth Powell, M.D., MPH. FACSM, was an epidemiologist with the CDC for 25 years and with the Georgia Department of Human Resources for 8 years. He is now retired and lives in Atlanta. The relationship between physical activity and health has been an important theme during his career. He planned, chaired, and edited the papers from the first national workshop on the epidemiologic and public health aspects of physical activity and exercise in 1985. Dr. Powell served on the Institute of Medicine Committee on Physical Activity, Health, Transportation, and Land Use (2005); Committee on Progress in Preventing Childhood Obesity (2008); and Committee on Physical Activity and Physical Education in the School Setting (2013). He was a member of the 2008 Physical Activity Guidelines Advisory Committee and a co-chair of the 2018 Physical Activity Guidelines Advisory Committee. He is a graduate of Harvard College, Northwestern University School of Medicine, and the Harvard School of Public Health.