Speaking with Michael Joyner, one feels as if one is sprinting to catch hold of a freight train. Formidable in both intellect and presence, Joyner sets the pace of the conversation, and you immediately feel as if you are an adoring but perhaps sub-par student. You daren’t fall behind — not because you are afraid but because you are in awe. At the very least, you want to see where the damn train is going; it will doubtless be both an interesting destination and a thought-provoking journey right along the way.
Fortunate, too, that Joyner’s own biography offers some hope for the supposedly sub-par student. More on this anon.
Joyner, recipient of the 2023 Honor Award of the American College of Sports Medicine, is the Frank R. and Shari Caywood Professor of Anesthesiology as well as departmental vice chair for research at the Mayo Clinic in Rochester, M.N. He’s received numerous awards and accolades, from the American Physiological Society’s Lamport Award for Contributions to Cardiovascular Physiology (1993) to an honorary doctorate from McMaster University (2019). He has well over 500 publications to his name. His Google h-index is more than 100, with upwards of 39,000 citations. He’s contributed articles and op-eds to, among others, Outside Magazine and The New York Times. He’s shared airtime with then-Vice President Mike Pence for his work treating COVID-19 patients.
Early days
But we start off the conversation at the beginning, so to speak. I enquire as to how he got into exercise science, and he recalls a case of serendipity. It was 1977. He was 19 years old and contemplating dropping out of the University of Arizona to join the fire department:
“I was the least prepared person ever to go to college,” he says. “I did well on tests, but I was a terrible student.”
In fact, Arizona was the third institution in which he’d enrolled, having beforehand tried his luck at both Earlham College and the Northern Arizona University, respectively. Really, the bright spot in his life was distance running — despite deep reservations about his place the academic world, he was a solid walk-on U of A track and field athlete.
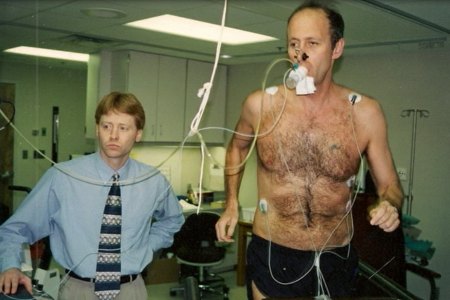 In this providential case, he was competing in a weekend road race when toward the end of the run he found himself keeping pace with a young graduate student named Eddie Coyle. Coyle was working in the lab of the legendary Jack Wilmore, a future ACSM president (1978-9) and Honor Award winner (2006). Coyle asked the younger runner if he wouldn’t be interested in becoming a subject in a human performance study headed by Pete Farrell, another grad student in Wilmore’s lab. Joyner agreed.
In this providential case, he was competing in a weekend road race when toward the end of the run he found himself keeping pace with a young graduate student named Eddie Coyle. Coyle was working in the lab of the legendary Jack Wilmore, a future ACSM president (1978-9) and Honor Award winner (2006). Coyle asked the younger runner if he wouldn’t be interested in becoming a subject in a human performance study headed by Pete Farrell, another grad student in Wilmore’s lab. Joyner agreed.
“Jack started letting me come to Journal Club and started letting me participate,” Joyner recalls, “because for some reason he realized that maybe I had some ability. And Eddie was super, super supportive.”
Later on in our discussion, Joyner shares, “I mean, I was barely 20 years old. The lightning bolt hit me and I said ‘I want to do this,’ right? And it was lucky because, you know, you didn’t have the Internet. There was nobody telling you this was stupid, or that it wasn’t possible, or that there would be some long and winding road.”
Eventually, with a diploma fresh in hand, Joyner followed Coyle to Wash U in the summer of 1981 to work with John Holloszy (the 1987 recipient of the ACSM Honor Award) on a study examining athletic detraining. Joyner, who had been in peak condition for his recent track season at Arizona, signed on as one of seven subjects and took a — presumably irritating — 12 weeks off so they could see what exactly would happen when high-level athletes potatoed from 60 to 0. The research eventually led to the 1984 publication “Time course of loss of adaptations after stopping prolonged intense endurance training” in the Journal of Applied Physiology: Respiratory, Environmental and Exercise Physiology.
But by 1982 Joyner had been accepted by the U of A medical school, where he found himself compelled by anesthesiology, particularly how well its basic components fit into his prior exercise physiology experience. He would go on to pursue anesthesiology for his clinical residency.
“The things you do in anesthesia — you think about breathing. You think about carbon dioxide. You think about oxygen. You think about blood pressure. You think about heart rate,” he says. “Those are the same things you think about during exercise.”
A career progresses
We go on to discuss the anesthesiologist’s role as the patient’s temporary autonomic nervous system, maintaining homeostasis while the patient is undergoing the physiological challenge of surgery.

As it relates to physiology: “We’re studying how this system works, how it’s affected by hypoxia, how it’s affected by exercise, blood loss, a number of other things I’m interested in. And in clinical anesthesia, we’re thinking about what happens when we turn the regulatory system off.”
However, Joyner is quick to delineate the realms in which he operates. He completed a clinical residency with extra research training at Mayo, expecting to stay a few years and then return to Arizona. Instead, he remained in Minnesota. Joyner’s current role at Mayo has him working as an anesthesiologist about 20 percent of the time. The rest is devoted to physiological research and teaching.
“Most of what I do is study humans in a clinical research center who are exercising, who we’re giving a different source of physiological challenges to,” he says, adding, “I’m an anesthesiologist thinking about physiology, but mostly what I am is a physiologist who also happens to be an anesthesiologist.”
And his research has delved into a fair number of seemingly disparate questions, from the causes of fatigue in subjects with cerebral palsy to the physiology behind world records. Joyner is himself a 2:25 marathoner, and many may recognize him as the name behind the 1991 physiological model that proposed the possibility of a sub two-hour marathon.
Naturally unsatisfied by narrow lanes of inquiry, Joyner is also instinctively suspicious of reductionism. His 2015 Times op-ed “Moonshot’ Medicine Will Let Us Down” presented doubts about the utility of precision medicine for the average person. The article caught the attention of Nigel Paneth, a pediatric epidemiologist at the University of Michigan, who reached out to Joyner via email. Together, they set up a network of researchers with varying fields of expertise but similar concerns about siloing in the scientific enterprise. “People who wanted to take a more broad-based, multifactorial view,” Joyner says.
COVID-19 and convalescent plasma
Through another series of happenstances, one of the experts in their group was Arturo Casadevall, an immunologist and microbiologist at Johns Hopkins University. In the early stages of the COVID-19 pandemic, Casadevall penned an article for the Wall Street Journal in which he proposed, based on a doctor’s inspired intervention during a 1934 measles outbreak, using the blood plasma of convalesced COVID-19 patients to treat those with an active infection. David Epstein, author of The Sports Gene, subsequently tweeted about the article. Joyner — who was at the 2020 Olympic Marathon trials to give a talk about his two-hour marathon research — saw the tweet, sensed momentum, and immediately emailed Casadevall.
Because of his anesthesia background, as well as some work he’d done with the U.S. Army, Joyner was familiar with the ins and outs of the nation’s blood-banking system. He thought they had a good chance of actually making this thing happen. He and Casadevall, along with other colleagues, set up sister research protocols at Hopkins and Mayo. By March 2020, Peter Marks, director of the FDA’s Center for Biologics Evaluation and Research, emailed Joyner about heading up an expanded access program for convalescent plasma. The effort treated more than 90,000 people early in the pandemic. As alluded to above, then-Vice President Mike Pence visited Mayo to hear Joyner’s update on the project. The meeting was broadcast on multiple national networks.
Of particular note, however, has been the effect of the plasma treatment on COVID-19 patients who also have leukemia or lymphoma.
“We’ve had patients who’ve had COVID for 300 days,” Joyner says. “Immunocompromised patients. This isn’t long COVID. These people have been actively infected, and they don’t get horrible COVID because their immune system is suppressed.”
We discuss the role of the inflammatory response, including cytokines. Then he floors me by saying, “So what happens is we’ve given these people a couple units of plasma and they get better right away.”
We move along, but later in the conversation he offers a generalist’s insight into the plasma program’s success:
“I think having a physiological perspective was helpful there,” he says, “as opposed to an infectious disease or microbiological or immunological perspective, just to be able to bring some outside thinking.”
Current and future efforts
 The convalescent plasma work is ongoing, but I ask about other irons he has in the fire. He rattles off a few ideas he and his teams are exploring, among them the effect of high altitude on exercise performance and working with people who are outliers on the continuum of physical health — particularly high-level athletes vs. those with heart failure vs. people who have left-shifted hemoglobin (i.e., those who possess a particular subset of hemoglobin that has a higher-than-average oxygen affinity). In this latter case, he’s interested to know whether humans with said unique hemoglobin perform better at altitude than the average person. Certain animals that inhabit or travel through dizzying elevations, including some geese that overfly Mount Everest, have similarly configured hemoglobin. It seemed worth looking into. Preliminary results suggest they’re onto something.
The convalescent plasma work is ongoing, but I ask about other irons he has in the fire. He rattles off a few ideas he and his teams are exploring, among them the effect of high altitude on exercise performance and working with people who are outliers on the continuum of physical health — particularly high-level athletes vs. those with heart failure vs. people who have left-shifted hemoglobin (i.e., those who possess a particular subset of hemoglobin that has a higher-than-average oxygen affinity). In this latter case, he’s interested to know whether humans with said unique hemoglobin perform better at altitude than the average person. Certain animals that inhabit or travel through dizzying elevations, including some geese that overfly Mount Everest, have similarly configured hemoglobin. It seemed worth looking into. Preliminary results suggest they’re onto something.
He’s also interested in what information might be gleaned from large datasets in an increasingly wearable-focused medical and fitness world. This work, however, remains in a “precognitive” state. It’s the second time he’s used the word during our conversation, and the repetition is telling. Joyner is a man who lets things work out organically, and in their own time. Or, rather, he doesn’t needlessly rush things. One recalls once more that he is a long-distance runner. There are moments you should push and times to let the road simply roll on beneath your feet. Press on, reflect, regroup, stay in a holding pattern. Everything in its season. We’ll get there.
“I’m sure we’ll make a lot of mistakes,” he says. “I’m sure there’ll be some false starts. But I think that if you see the mountain peak 50 miles away, it looks pretty good.”
“Since Dr. Joyner attended his first ACSM meeting four decades ago, he has helped establish and solidify ACSM as a world leader in exercise and physiological science and medicine. I respectfully submit that it is loyal, ethical and supremely gifted individuals such as exemplified by Dr. Joyner that have helped make our organization what it is today.”
- Honor Award nominators Timothy I. Musch, Ph.D., FACSM and David C. Poole, Ph.D., FACSM